Your Jaw Tension Is Treatable. Here Is What Botox for TMJ Actually Does.
Jaw pain, grinding, and morning headaches are treatable with Botox. The aesthetic benefit is a bonus most men do not expect. Here is the clinical picture.
Elena Gorbunova
PA-C, Beauty Medica

- TMJ dysfunction and masseter hypertrophy are medical conditions, not stress habits you manage away.
- Botox injected into the masseter interrupts the clenching cycle, reduces pain, and often produces a more defined jaw as a secondary effect.
- Relief begins in three to five days. Most men maintain every three to four months.
- Botox for TMJ is an off-label but well-documented application supported by peer-reviewed clinical evidence.
The problem that builds over decades
TMJ dysfunction is one of the most undertreated conditions I see in male patients over 50.
By the time a man is in his mid-50s, he may have been clenching and grinding for twenty or thirty years. What started as occasional jaw tension has become structural. The masseter muscles, the paired muscles that power chewing and clenching, have hypertrophied from decades of chronic overuse. The joint itself has accumulated wear. The symptoms, jaw pain, morning headaches, and teeth grinding, have become the baseline.
Most men manage it. They take ibuprofen. They buy nightguards. They tell themselves it is stress. When they finally come in, it is often because the pain became impossible to ignore, or because a dentist flagged the masseter size on an X-ray.
The good news: Botox for TMJ is one of the most evidence-backed functional applications of neurotoxin therapy, and the aesthetic benefit, a more defined jaw as the muscle reduces, is a bonus most men appreciate once they experience it.
What TMJ dysfunction is
The temporomandibular joint connects the jaw to the skull. TMJ dysfunction covers a range of conditions causing pain, tension, and mechanical problems in this joint and its surrounding muscles.
In men over 50, the most common driver is masseter hypertrophy from chronic clenching or bruxism. This is not a habit you discipline away. It is a physiological pattern that, once established, continues independently of conscious effort. The muscle keeps contracting. The clenching cycle continues. The symptoms persist.
Symptoms include:
- Jaw pain, most pronounced in the morning or after periods of stress
- Headaches originating at the temples or along the jaw
- Tooth grinding during sleep, often reported by a partner before the patient recognizes it
- A persistent sense of tightness in the face and jaw throughout the day
- Premature tooth wear documented on dental examination
- A wide, squared lower face from muscle overdevelopment
How Botox treats it
Botox injected into the masseter muscle blocks the nerve signals that drive involuntary contraction. The muscle cannot clench at full force. The grinding cycle is interrupted. Pain diminishes as the muscle is no longer contracting repeatedly against a fatigued joint.
Published research supports this mechanism. A clinical study in the Journal of Oral and Maxillofacial Surgery demonstrated significant reduction in pain scores and jaw tension in patients treated with botulinum toxin, with effects sustained across the treatment period. A separate review in the Journal of Clinical and Diagnostic Research confirmed meaningful clinical improvement in TMJ pain outcomes with botulinum toxin compared to control groups.
The neurotoxin metabolizes over three to four months, which is why maintenance treatment is required. In that window, the jaw resets. Many patients find that with consistent treatment over time, the baseline severity of clenching decreases.
The treatment itself:
- Takes 15 to 20 minutes total
- Involves small injections into the body of the masseter, on both sides
- Requires no anesthesia for most patients
- Has no downtime
The aesthetic benefit men do not expect
Here is what most men do not anticipate: the masseter reduces in volume over four to six weeks as the muscle stops working at full force.
For men whose jaw appears wide or squared from masseter overdevelopment, this produces a meaningful aesthetic change. The jaw becomes more defined. The face looks sharper. The transition from jaw to neck reads more cleanly.
By the 50s, many men are dealing with both masseter hypertrophy making the lower face heavy, and volume loss higher up the face creating hollowing. The combination reads as bottom-heavy and fatigued. Treating the masseter addresses both the pain and the lower face proportion at the same time.
This is not the primary goal of TMJ treatment. It is a consistent secondary benefit that most male patients choose to maintain.
What to expect
Timeline:
- Jaw tension begins reducing within three to five days
- Grinding frequency typically decreases in the first two weeks
- Full pain relief noticeable by two to three weeks
- Masseter volume reduction occurs over four to six weeks
Duration: Three to four months for most patients. With consistent treatment, some extend to five to six months.
Downtime: None. Minor tenderness at injection sites for 24 to 48 hours is normal. Normal activity resumes immediately.
Common questions
Is this FDA-approved for TMJ? Botox is FDA-approved for several indications. Masseter injection for TMJ is off-label, meaning the FDA approved the product, but not specifically for this application. Off-label use by a qualified provider is standard in medicine and reflects established clinical evidence, not experimental practice.
Will this change how my jaw looks? For men with an overdeveloped masseter, yes. The jaw often becomes more defined as the muscle reduces. For men with a normally developed jaw, the visible change is minimal.
What about a nightguard? A nightguard addresses mechanical tooth wear. Botox addresses the muscle force driving the grinding. Many dentists recommend both in combination. They work through different mechanisms and are not mutually exclusive.
Does it work alongside other treatments? Many men combine TMJ treatment with facial neurotoxin or structural filler in the same session. The treatments complement each other and are often planned together.
- Patel J et al. Efficacy of botulinum toxin in treatment of temporomandibular joint disorders. J Clin Diagnostic Res. 2017
- Shim YJ et al. Botulinum toxin injection for chronic temporomandibular disorder. J Oral Maxillofac Surg. 2014
- FDA: Botulinum toxin approved uses and safety information
- American Academy of Orofacial Pain: Clinical Resources
Elena Gorbunova
PA-C, Beauty Medica
PA-C, Beauty Medica
Related articles
Continue with another article from this section.

Why Aesthetic Results Depend on Shared Vision, Not Just Products
The same tools can create very different results. Patients should choose a provider whose aesthetic vision aligns with theirs.
Read article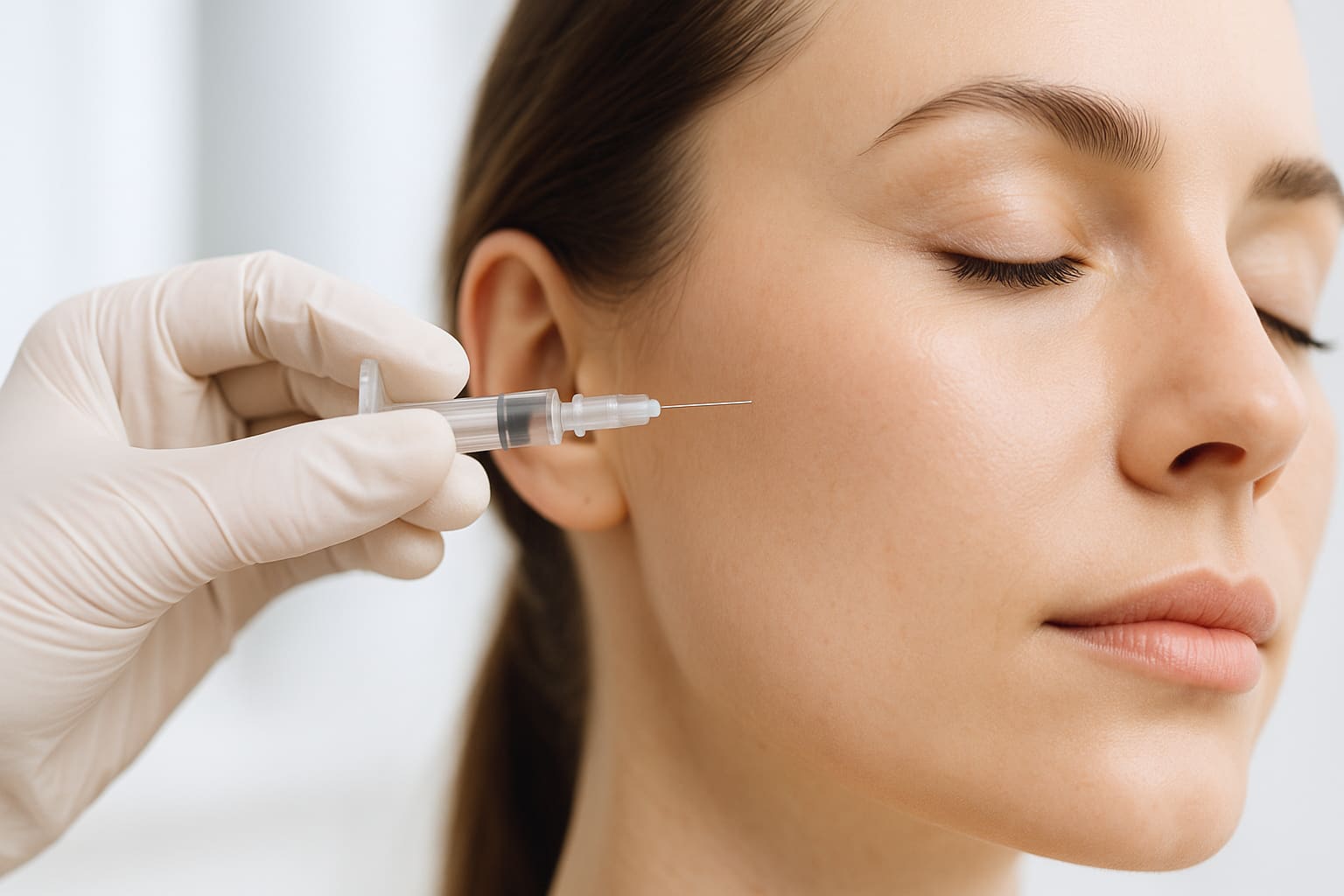
Skin Boosters and Exosomes: What They Are, What They Are Not, and What to Ask First
Patients often arrive with a search term. This guide explains how skin boosters, exosomes, Gouri, and related treatments fit inside a broader Skin …
Read article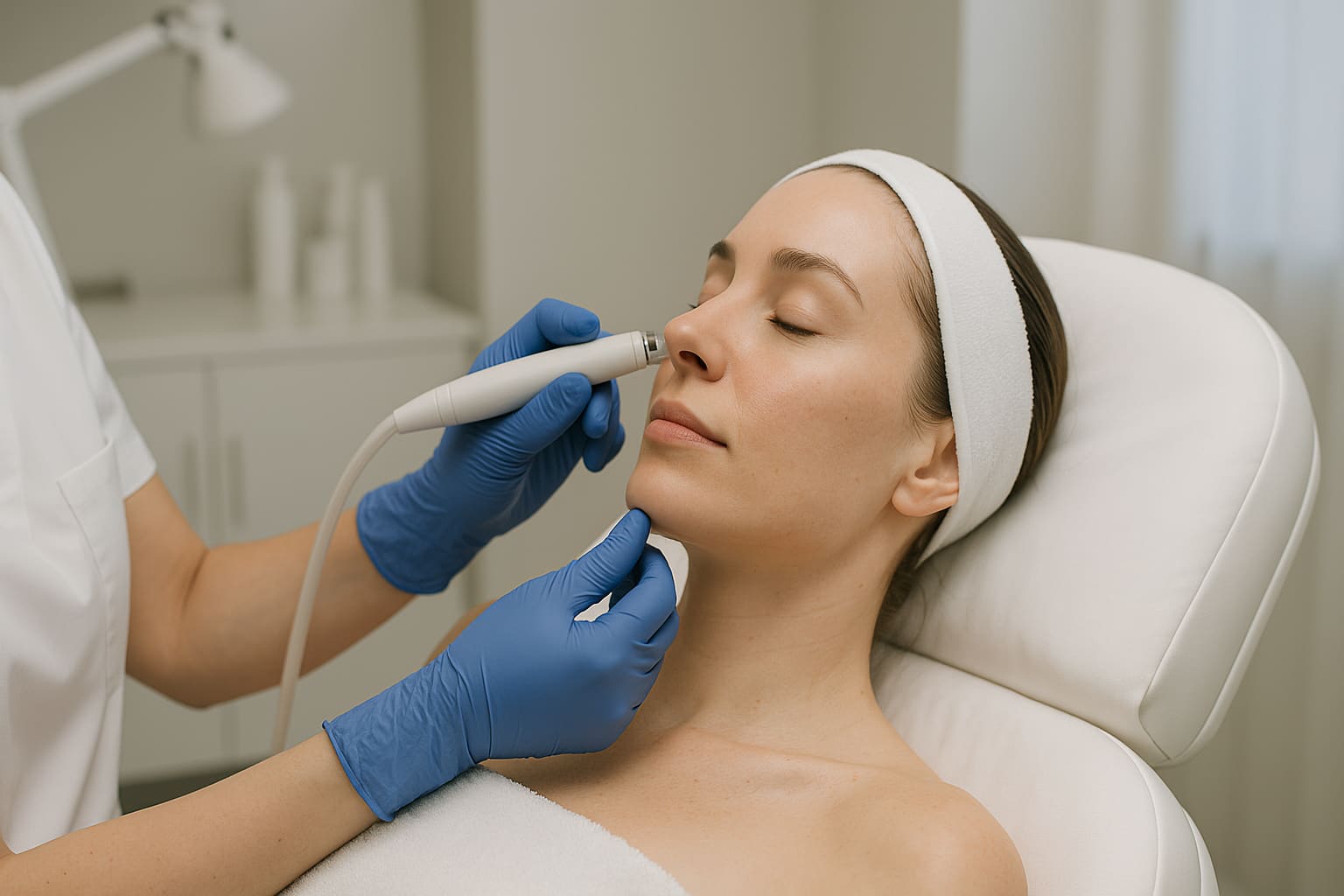
Your Skincare Routine Did Not Fail. Your Hormonal Environment Changed.
When hormones shift, skin behaves differently in ways your routine no longer addresses. Here is what is actually happening and which clinical …
Read article